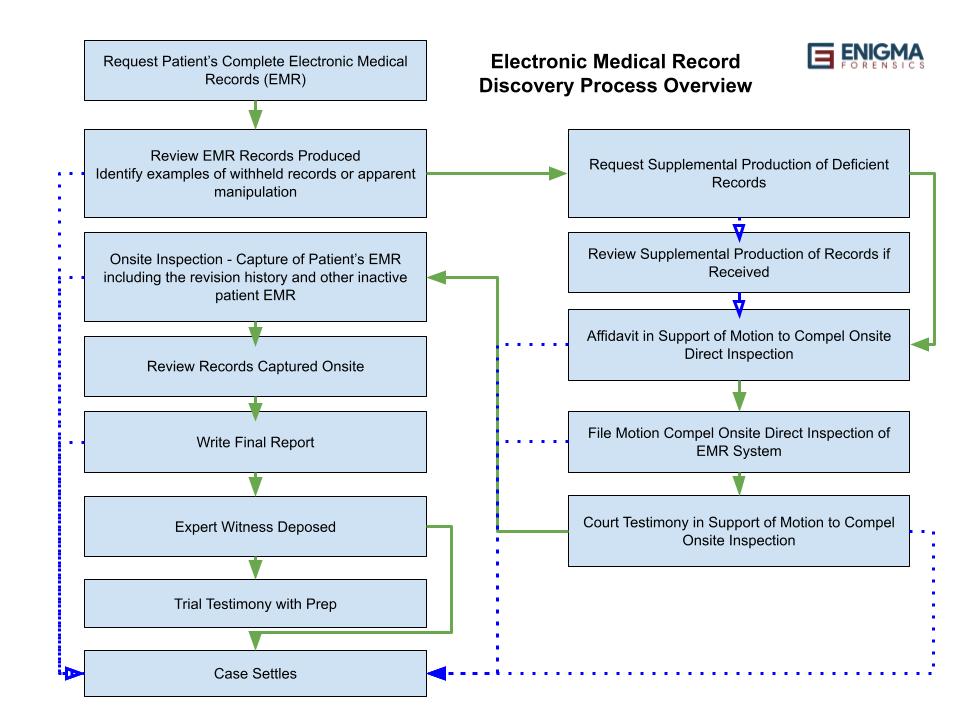
Process of Navigating to Trial or Settlement
Lee Neubecker: So now I’m going to a little bit about the overview and process of working one of these cases with electronic medical records, such as myself. And typically, the cases start off with the need to make the request for the complete electronic medical record. Oftentimes, attorneys contact us when this has already been done but they suspect that the data is deficient in some way or fabricated.
So, we often will review the records produced, identify examples or problems with filters, anything that looks suspect, and then assist with drafting a supplemental request to produce.
If the supplemental materials are produced, we review that. We look for deficiencies in the records, and oftentimes there will still remain deficiencies. So in that case, we have to spend time analyzing the EMR and working on a report of sorts that shows examples of what’s missing. And at that point in time, we’re trying to compel the judge to order an inspection. On the converse side, if we’re working for the hospital, we’ll be looking through the EMR and often reporting to them whether or not there was a fabrication by hospital staff and that’s important for insurance carriers because they want to understand what the risk is if they litigate a case to trial. And it may be more advantageous to simply settle the case if there are some problems in the EMR.
So after we’ve drafted the motion to compel, well, typically, we write an affidavit in support of the motion to compel an onsite direct inspection. That motion gets filed by the attorney with our affidavit attached and then there’s a hearing. These days, the hearings tend to be on Zoom telephonically, and oftentimes the judge will ask questions. Essentially when we’re doing an onsite, what we want is we want to be able to see the entire record of the patient as the physician can see it, the communications between providers, and the complete revision history. This often requires videoing or taking photos of the data to capture data that are not easily printed from current reports with the HIS system.
So when the onsite inspection happens, it’s not uncommon that there will be multiple experts there. I’ve been hired to observe an inspection by a plaintiff counsel that is seeking to look at the EMR. In that role, I’m looking to just document and understand how they’re requesting the data, whether data is being withheld despite the onsite, and to advise my client in terms of what the data is that was produced and whether there are any issues with it. The onsite inspection isn’t where the analysis happens. It’s usually an effort to try to dump all the data out, run reports, make sure the settings are documented appropriately, and really that the only filter being used is the filter for the patient. There should be no other need to filter anything. Those records are the patient’s records. They have a right to that content and this process is one that is going to become much more common as we continue with the understanding of medical records and audit trails becoming more prevalent. After the onsite inspection, there’s a need to review that data. Oftentimes normalize it again, compare it against earlier produced EMR. That analysis might document that early on, that the health care organization was willfully holding back information that was key and important. And so, in instances where that happens, there’s a need to write a report to document those changes or deficiencies. And long before the trial happens and the reports issued, the expert witness that you use is your EMR expert will have to be deposed most likely. And what I usually find, at least in cases I’ve been involved with is that the cases typically settle after the deposition. Because at that point in time, you’re really looking at what does the factual record reflects? There are not so many opinions so much as there are facts. In some cases, there are opinions about why does the chart shows lots of entries that all were created days after discharge and they’re all unrounded hours with no minutes. In a situation like that, my opinion would be that’s likely fabrication because usually if you’re entering notes and other procedures contemporaneous to events, you’re going to have randomization of the minutes and everything is not going to be stacked up at zero, zero minutes on the hour.
So if a case is going to trial, there’s a need to prep your EMR expert, to let them review the timeline, the earlier affidavits in the data that was collected so that they’re prepared for trial. In most cases, so cases tend to settle and they usually settle after the onsite inspection and collection of data. Sometimes they’ll settle much earlier. I’ve seen cases settled as soon as I get involved and help with writing a request for supplemental production but sometimes the cases go on further. In my experience, the further along through this process the plaintiff gets, if we’re able to identify willful withholding of records, the settlement offer tends to be much higher.
1. Request Patient’s Complete EMR
- Provide the complete EMR audit trail for [Patient Name] detailing any health care provider’s access, review, modification, printing, faxing, or deletion activities in a comma delimited format with any and all corresponding native files or records that may relate to the patient as required by the HIPAA § 164.312(a)(1).
- Audit trail should include the complete revision history of the EMR
- Provide the name of all medical software applications utilized to store EMR
- Provide the data dictionary for each software application containing EMR
- Provide all User and Administrator Manuals for each EMR software application
Email [email protected] for a complimentary sample request for EMR
So, I gave an overview of this. There are slides here that I’ll walkthrough. I want to have plenty of time for questions. So, I’m not going to read each of these but in summary, you want to make sure that you’re getting all the data and there’s an outline here, if you email [email protected], she can send you a complimentary sample request for EMR that helps you form that request. Obviously, you may want to retain us to help you tweak that for your specific circumstances. It’s a good idea though to ask for the user manuals when you’re doing this process and you want to make sure that you’re clear about asking for the complete revision history.
2. Review EMR Records Produced
Identify Examples of Withheld Records or Apparent Manipulation
- Filters beyond the patient used such as user id or department
- Lack of production of records from the beginning of the notable time period until the date the EMR report was generated
- Audit trail lacks details of the revision history
- Production of the data in a non-usable format
So I talked about the review of the records produced and typically, we’re trying to identify examples of withheld records or other things that we can find or prove that are deficient from the production. Audit trails that lack the definition of what was being changed are an example, the production of data in a non-usable format, going onsite to have it exported. So it’s not produced in a crazy, out-of-order duplicative format is often helpful.
3. Request Supplemental Production of Deficient Records
- Ask for what you want specifically before filing a motion.
- Request the complete revision history showing the life cycle of the patient’s EMR.
- The supplemental request for the production of deficient records is likely to not bear fruit but is necessary to show you tried to work things out before seeking judicial intervention.
So when we’re asking for the records that we’re missing, we want to be specific on that and ideally pose that directly to opposing counsel in an email. So that it’s documented and that way, if you’re hearing a motion, you can show the judge that you’ve already tried to be specific about what you were asking for. It should always include the revision history. That phrase is so important. Usually, that’s missing from productions. And it’s often, the case that even though you ask for things correctly, they still aren’t produced as requested. So, having that clear documentation of asking for it in email is important.
4. Review Supplement Production of Records Received
- Immediately review the supplemental production upon receipt.
- Check to see if the request that was made was answered correctly.
- To the extent that production remains unresponsive, communicate that to opposing counsel before filing your motion.
So when the supplemental production comes in, we want to typically look at that quickly, try to see if they’ve complied or failed to address certain sections. If they failed to disclose their filters or they filtered things differently than requested, you want to create a paper trail and send a follow-up email asking for that, and then if they don’t comply, that’s going to help you with your motion to compel when appearing in front of the judge.
5. Affidavit in Support of Motion to Compel Onsite Direct Inspection
- Detailed foundation for the request
- Reference prior requests and data produced
- Communicate the deficiencies in the produced EMR
- Establish examples where the revision history showing changes is important
- Establish that the reported dates are not necessarily the original entry time and that modification history can be obtained by directly examining the EMR system
So the affidavit that we’re generating is typically outlining these deficiencies. It might be sharing exhibits that include the emails that you sent asking for the data. We want to make sure that we’ve detailed the foundation for the request, pointing out examples of what was asked for what was produced, how that was deficient? Giving examples where the revision history showing changes is important. Specifically, the lack of when the records were actually created or last updated, who updated them, when? That information is very important and it’s often not in the initial round of production of EMR.
6. File Motion To Compel Onsite Inspection Of EMR
- A federal U.S. District Court ordered a hospital to provide such direct access to a patient plaintiff in a medical malpractice case. (Borum v. Smith, W.D. Ky. No. 4:17-cv-17, 2017 U.S. Dist. LEXIS 109249 (July 14, 2017)
- The court’s decision lays out the arguments made by the hospital opposing the onsite inspection.
- https://cases.justia.com/federal/district-courts/kentucky/kywdce/4:2017cv00017/101673/31/0.pdf?ts=1500121148
So, finally the motion to compel the onsite inspection of EMR, there’s a useful case out of Kentucky, Western District of Kentucky, the Borum versus Smith case. I think on our website, if you search at enigmaforensics.com for Borum, B-O-R-U-M, there’s a hyperlink to this case and it’s a federal case that lays out the arguments establishing and overcoming objections made by a hospital resisting an onsite inspection. So this can be very useful to lay the groundwork for arguing your motion to compel.
7. Court Testimony in Support of Motion to Compel Onsite Inspection
- Having your EMR expert at this hearing is important
- Overcome objections
- Establish protocol for examination
- Allow recording of the HIS software as it relates to the patient
- Allow for the reproduction of previously produced EMR to verify filter settings and obtain the data in a delimited format
- Ensure that all versions of notes including inactive and historical versions are included in the production of EMR
When that motion to compel hearing is held having someone like myself there to be able to answer questions of the judge, overcome objections, help to establish protocols for the exam to ensure that it’s effective and not a waste of everyone’s time is important. Recording of the HIS software should be allowable. An agreement to redact or call out anything that might’ve been captured that doesn’t relate to the patient is something that I see there’s no issue to but the ability to document and the record is critical. Ideally, during this onsite, you want to be able to reproduce what they produced previously so that you can confirm whether or not they had filters applied to it. If their earlier production of EMR only includes active records and no historical records, producing it in a more complete manner will help you to demonstrate to the court that the hospital was holding back important records that were your patient’s or your client’s records, that they have a right to. So again, making sure that inactive historical versions are included in the production of EMR is very important.
8. Onsite Inspection – Capture of Patient’s EMR
- Inspection can occur using Zoom or other remote desktop tools
- An in-person inspection can be advantageous
- Your EMR expert should be able to direct the health care provider’s IT admin to perform any query or other activity that relates to the patient
- Data can be saved to external media for later examination
- Your EMR expert should be allowed to capture photos or video from the live system
So inspection onsite during the pandemic, a lot of things have shifted to Zoom or WebEx, that can certainly happen. An onsite inspection does have advantages and I usually recommend the onsite where possible. Now that vaccines are widely available, the concerns over going onsite should be much less. During this inspection, I always recommend that the healthcare providers, IT person with admin rights actually be the person that’s typing at the keyboard and moving the mouse but at the direction of the requesting party. That helps protect from any potential harm to the hospital information system and really shuttle out for full observation of the EMR as it exists within the system.
Typically, data is exported to external media and at the conclusion of that, the data is shared with a producing party, in requesting party subject to the right for either party to deem data confidential or redact, which typically, the confidentiality requirements, hospitals are already following that for the most part. So really, as long as the data is restricted to the patient, there really shouldn’t be much reason to hold back data that belongs to a patient as long as it’s just that patient’s data. That data will be examined after the onsite when there’s time to analyze it.
9. Review Records Captured Onsite
- Limited time for onsite inspection and collection of data
- Consider delaying review if a settlement offer is likely
- EMR expert compares initial productions vs. onsite data collected
- Identify examples of manipulated records or previously withheld records
- Consider disclosing some of these smoking guns before proceeding with a written report by an EMR expert
So after the onsite, that’s when there’s more time to look at the data to analyze it, to compare it. If there’s an expectation that smoking guns were captured during the onsite, sometimes a plaintiff expert might want to just hold off for a week or two if they think that a settlement’s likely so that the costs aren’t incurred. To discuss the comparison of initial productions versus what was collected on-site, trying to identify examples of manipulated records or previously withheld records can be important in understanding what happened with the case.
So whether or not you write a formalized report or just disclose some of the smoking guns, that’s a decision that plaintiff counsel often considers. Defense counsel often needs to consult with their insurance carrier and have someone like me help tell them what the situation is so that they can decide, does the case have merit or should you proceed to trial and not make a settlement?
10. Write Final Report
- Detail examples of previously withheld information
- Detail examples of fabrication or manipulation of information
- Clarify what happened with the EMR
So the final report that gets written up again, details, examples of previously withheld information. Examples of fabrication or manipulation of information and trying to clarify, in human words, a storyline of what took place.
11. Expert Witness Deposed
- Survive Daubert challenge
- Avoid mistakes
- Establish a foundation for the admissibility of electronic evidence
- Clarify any opinions expressed in the affidavit(s) or report(s)
So, when the deposition phase occurs, it’s important that your expert be able to survive a Daubert challenge. You don’t want to have all the work tossed out because the collection of data was not done properly or not performed by someone that has appropriate experience. It’s important to try to avoid mistakes, which sometimes typos happen and whatnot but trying to minimize mistakes typically requires giving your expert time to review and proof their report. Having other peer review processes performed and engaging with your expert to make sure that everything is clear and understandable. And ultimately, you’re trying to establish a foundation to admit important information that relates to EMR so that you can clarify what events took place and having your expert be able to explain that to a judge is really important.
12. Trial Testimony with Prep
- Select an expert that is skilled at presenting technically complex information to non-technical audiences.
- Verify that your expert has court testimony experience.
- Ensure your expert has time to review materials before trial.
- Most cases never make it to trial and settle earlier where the EMR speaks for itself.
So one of the things you want to look for when you’re picking an expert, you want to look for identifying an experienced expert that has testified on cases before and is capable of taking technically complex information and presenting it in an easy-to-understand manner. And that isn’t always easy for many geniuses out there that understand a lot of complex information. You want to make sure again, that your expert has time to refresh and review the materials before trial. Experts that are busy are going to be in many different cases and shifting between one med mail case matter in another involving EMR takes some time to shift.
So, I like to try to work on a case solidly for a period of time, get it up to a report, finish that and then come back to a case at the next checkpoint so that I can focus and not be split between two similar but different cases. As I said before, most cases never make it to trial because ultimately, the electronic medical records, if obtained and produced in their entirety with the date and time that they were entered, modified, and whatnot, that data will typically speak for itself. So, whether you’re defending a case or pursuing one, getting an understanding of events that took place, it’s highly critical.
13. Case Settles or Case Dropped
- In our experience, in cases where EMR has been withheld or manipulated, settlement agreements are usually reached.
- Establishing that the medical record doesn’t support allegations of abuse can result in a case being dropped.
- Settlement offers increase when you are able to prove that the health care provider purposely withheld information.
- Proving willful fabrication or manipulation of the EMR can help win the highest settlement.
So when we find examples of manipulation of information, settlement agreements are usually reached because if a hospital took a case to trial and it was proven that they manipulated the records, they would face far more litigation from other plaintiffs as a result of that. In some cases, some of the outcomes might not be to have a cash settlement, it might be for a parent to regain custody of their child because there were inappropriate allegations of harm that aren’t substantiated by the electronic medical record. If you can prove that a healthcare provider purposely withheld information, it’s really helpful to get a settlement or a favorable outcome if you’re on the plaintiff’s side. And again, as I said, what I’ve seen is the highest settlement offers usually come if you prove the willful fabrication or manipulation of EMR.
I had a case back in, I think it was around 2004 involving a heart catheterization operation that went wrong, and days after the operation, the patient was discharged and then passed away. It’s an unfortunate circumstance that left a family with one less parent. In that case, so years after the accident, the surgeon produced a CD disk that contained the video clips documenting the surgery. But what happened when I examined the CD, I was able to establish that the CD had been created a month previously. The CDs have headers that show the date and time that they’re created by a specific computer.
Furthermore, I looked at the video clips, there were DICOM video files. DICOM is digital imaging and communication of medicine and these video files had embedded metadata that showed the sequence number and the date and time and length of the clip. Well, what had happened is I think it was clip six, seven, and eight were deleted nine, 10, and 11 were renumbered to be six, seven, and eight. So there were three video clips that were removed and then the renaming of the files effectively made it look like the deleted clips never existed. Well, in doing forensics on that, I was able to establish what had happened and then during my deposition, I testified to that. At the end of it, the attorney for the hospital asked me, do you have any proof that the hospital had anything to do with this? Keep in mind, the surgeon was the one who produced the CD years after the operation.
Oh, my reply to the attorney for the hospital was if, given the opportunity to examine the hospital’s equipment, I could determine whether or not the CD that was produced was generated by their equipment and my deposition ended. Quickly after that, they asked for my business cards and then the maximum settlement of the insurance coverage from both the surgeon and the hospital, that offer was made in the case of, so it was a favorable outcome.
One other thing too, in many cases that have caps on liability, if the plaintiff is able to prove willful manipulation, in some states, those caps go away. So, if you’re defending a hospital in one of these cases, having someone like myself help you determine if the EMR shows willful manipulation or fabrication. That can be very important because exposure to the hospital could be much greater than in the case where things simply, you know, mistakes happen and unfortunately, mistakes happen and good people suffer harm as a result of disease, surgeries, and whatnot. But in situations where bad things happen and then individuals in a healthcare organization take efforts to fabricate the record, to make it look other than what events really took place, that can be very risky for a healthcare provider. And knowing that early on in a case is really important that hospitals know that and other health care providers. So in those situations, I’ve had a lot of experience digging in and answering those questions quickly before the plaintiff gets their answers. I’ve also helped the plaintiff get the answers to those questions and reached satisfactory settlements.
Watch other videos making up this 4 part series, Unlocking the EMR Audit Trail.
| Part 1 of 4: “The Keys to Unlocking Electronic Medical Records” https://enigmaforensics.com/blog/keys-to-unlocking-the-emr-audit-trails-electronic-medical-records/ |
| Part 2 of 4: “HIPPA” https://enigmaforensics.com/blog/health-insurance-portability-and-accountability-act-of-1996-hipaa/ |
| Part 3 of 4: “Navigating to Trial or Settlement” https://enigmaforensics.com/blog/navigating-to-trial-or-settlement/ |
| Part 4 of 4: “In-Person Direct Access” https://enigmaforensics.com/blog/in-person-direct-access-provides-additional-information/ |